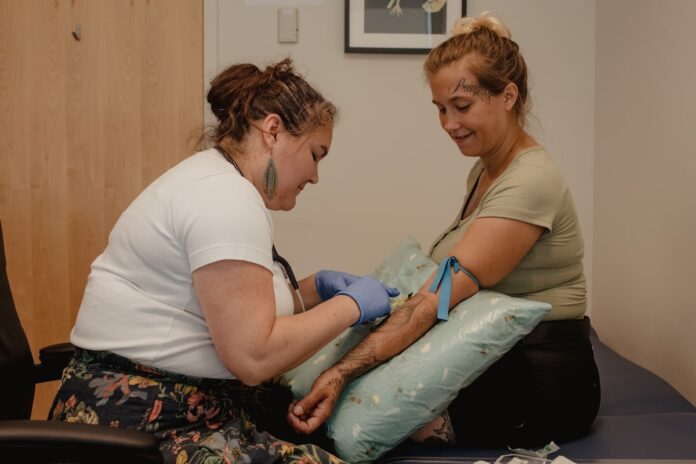
In the early days of the COVID-19 pandemic, fear was rampant and information about the virus was scarce. As concerns grew about the heightened risk indigenous communities faced, a group of dedicated health workers sprung into action. A phone line during the pandemic that morphed into a clinic providing culturally safe care in downtown Toronto was launched, staffed by Indigenous midwives and community health workers who came to be fondly known as “aunties”. This initiative was spearheaded by Cheryllee Bourgeois, a Métis midwife, and her team.
Addressing the Crisis and Beyond
The Aunties’ initial response was to launch a phone line in April 2020, dubbed the Call Auntie hotline. The line was staffed for four hours every day to provide advice and support to Indigenous patients. The team also addressed broader issues such as housing, embodying the Indigenous values of kinship and care.
“The idea was ‘Who do you call when you’re worried, trying to figure something out?’ You call your auntie to talk it through,” Ms. Bourgeois explained. By August, the hotline evolved into a physical clinic offering in-person care, including sexual and reproductive health services. The clinic, which operates once a week at the Toronto Birth Centre, provides a range of services, from diagnosing lumps to providing diabetes medication.
Creating a Safe Space for Indigenous Health Care
The clinic is more than a health center. It’s a community hub where staff look after children while their parents attend appointments, and where a talking circle called ‘All About Our Relationships’ is held. It is a space designed to reduce the barriers Indigenous people face when accessing health care services.
Given the persisting concerns about anti-Indigenous racism in health, the importance of safe and culturally appropriate health care cannot be overstressed. Many Indigenous patients express fears about the treatment they might receive in conventional medical facilities.
The tragic case of Joyce Echaquan, a mother of seven who endured racist taunts by health professionals while seeking help at a hospital, underscores these fears. A coroner’s inquest found that a combination of systemic racism and health system failings contributed to her death, further emphasizing the need for safe, Indigenous-led health facilities like the Call Auntie clinic.
Indigenous Leadership and Community Commitment
Among the clinic’s leaders is Suzanne Shoush, a First Nations and Black doctor who is also the Indigenous health faculty lead at the University of Toronto. The Indigenous Physicians Association of Canada applauded the progress of the Call Auntie clinic, describing it as “a full wrap-around care model grounded in Indigenous ways of knowing, being, and healing.”
Ms. Bourgeois stated that the clinic collaborates with community organizations, like the Inner City Health Associates, to offer services to people living in precarious housing conditions in Toronto. She shared the example of a client who lives in a tent and was assisted by the clinic to access and recover from surgery.
More Than Just a Clinic: A Place of Kinship and Care
At its heart, Call Auntie is about relationships and community. It offers a place for people to gather, share, and support each other. Homemade soup and comforting cups of tea are always available, symbolizing the warmth and care that permeates the clinic.
“We really think of the people we interact with as our relatives and we draw on the teachings that we have about how to take care of each other,” Ms. Bourgeois said. In a world where health care can often feel cold and impersonal, the Call Auntie clinic stands as a beacon of compassion, kinship, and culturally sensitive care.